Thursday April 21, 2022 – Another day to add to my timeline in this battle. After 4 years of clear scans, my progression free survival (PFS) on Alectinib as a first line treatment is 52 months. Something felt off all day on that Thursday when I had my routine scans and appointment at UVA.
After having 16 CT scans since starting this journey, I knew what to expect walking into each. There is a certain chill I’ve come to anticipate during the scan and this time, the chill was delayed. When we were called in for my appointment with Dr. Hall, the wait in the room seemed longer than usual. I knew something was off when he entered the room. Usually, when Dr. Hall enters the room the first thing he says is “your scans look good”. This time he asked “how are you feeling?”. He pulled up my most recent and past CT scans and it revealed an area above the original tumor site in the lung that has started lighting up brighter over the past 18 months. In past scans, it has appeared as ground glass, but this time there was definitely something more substantial.
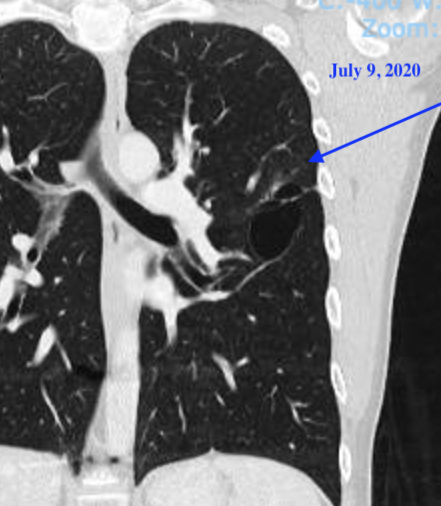

Just to be sure we decided to have Dr. Hall present my case at tumor board the following week where the oncologist, radiologist, radiation oncologist, and thoracic surgeon specializing in cancer meet weekly to discuss unique cases. It was a long weekend of waiting to hear back and finally on Tuesday night, I received a call from Dr. Hall. After looking at the scans from different angles, they confirmed that something was changing and it was concerning in the upper left lobe of the lung. Initially at my appointment, we had discussed radiation; however, after reviewing the scans at tumor board, they discovered there were spiculations coming out of the lesion that the radiation may not be able to completely eradicate. After a long conversation about options, I asked Dr. Hall what he would if he were in my shoes and he said he would surgically remove it to ensure we got it all. This would also allow us to test the tissue to see what type of resistance the tumor may have acquired. Similar to COVID and other viral diseases, the cancer cells are being kept at bay by the medication I take everyday but over time the disease always wins and develops a new mutation that outsmarts the medications. The goal of surgery would be to remove the cells that have figured out how to beat the medication in hopes of continuing the same treatment regimen. This is important because there are not very many options after this pill and would likely lead to a chemotherapy, which has not been shown to be as effective as the medications I currently take.
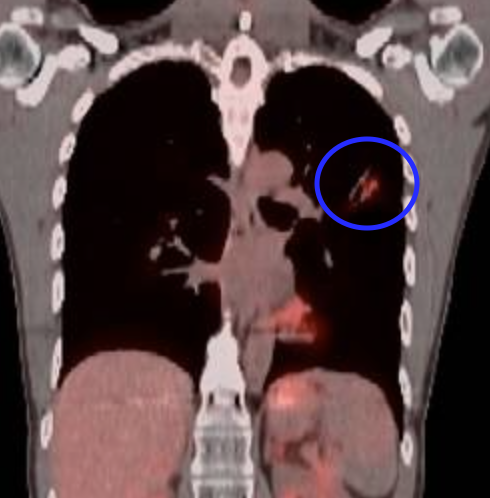
After my phone call discussion with Dr. Hall came the marathon of scans and appointments the following Wednesday. I had an MRI on the brain and PET scan of the rest of the body to determine if this was oligoprogression, a state where a single/few lesions display further progression after an initially successfully systemic therapy. Fortunately, the scans confirmed there was only the single spot of progression in the lung and after another appointment with Dr. Hall to review the scans, we elected for surgery as the next course of action. I also had blood taken for a liquid biopsy with Guardant, which tests your blood for circulating tumor DNA to allow for molecular analysis to understand if there are specific targetable mutations for better treatment planning in the future.
Next, I met with Dr. Linda Martin, a thoracic surgeon at UVA. She works with Dr. Hall on the tumor board and was highly praised by other surgeons within her field. After speaking with her about the procedure, we decided to move forward with scheduling the surgery to remove the upper left lobe, which is quite a large chunk. I was expecting to have minimally invasive surgery so that my recovery would be quick and the incisions would be small, but due to the previous history of cancer in my chest there was concern that too much scar tissue would be present. The scar tissue would have made it difficult to adequately remove the cancer and surrounding lymph nodes with only a minimally invasive approach. This means I would be having a more aggressive open approach, thoracotomy, to remove the left upper lobe of my lung. Since I was already at the hospital, I also completed my pre-anesthesia evaluation for the surgery. It was a very long day, but I was glad to come out of it with a very clear plan. Next up, I have a pulmonary function test scheduled for 5/19 and then the big surgery will be on 5/26.
I knew this day would come at some point because we still haven’t been able to figure out how to stop the disease from outsmarting the targeted therapies. I was hoping that it wouldn’t have occurred as soon, but I am very grateful to have beat the average PFS for Alectinib of 34.5 by almost 1.5 years. I have also seen great success continuing on Alectinib following targeted removal of oligoprogressive lesions from other ALK positive survivors and am hopeful that removing this one spot will allow me to continue on the Alectinib for many more years.




After 2 long weeks, I was able to take my mind off of everything that was going on with my health and reconnect with many of my colleagues at the wedding of one of my fellow OMFS attending’s (and former co-resident), where I was a groomsman and Avery was the flower girl. We were so honored to be part of the celebration for Drs. Daniel and Annie Hawkins.
Everyone has hiccups and speed bumps that occur throughout their life. But these hurdles that occur shine light on the many things that I am thankful for. I have co-workers and a department that have been so understanding and have made sure that I have as much time as I need to heal and recover. I have friends and family that have shown so much support and love as I shared this terrible news. I have the most amazing wife who has stood by my side and been my rock as I weather this storm. In case I don’t say it enough, thank you all for everything. It has been a very tough few weeks (to say the least), but for now I will continue to live life one day at a time and savor every moment!
